Symptoms
What Are the Symptoms of Congenital Sucrase-Isomaltase Deficiency?
The clinical presentation of Congenital Sucrase-Isomaltase Deficiency (CSID) can vary from mild to severe chronic, watery diarrhea and/or abdominal pain.
In This Section
Often, symptoms do not manifest in infants until they begin to ingest sucrose and starch-containing foods (for example, juices, solid foods, and medications sweetened with sucrose).
Chronic, watery diarrhea and failure to thrive are the most common symptoms in infants and toddlers. Other manifestations include abdominal distention, gassiness, colic, irritability, excoriated buttocks, diaper rash, and vomiting.
In some populations, notably the Greenland Eskimos and some Alaskan natives, a low-carbohydrate, high-protein, high-fat diet may delay the development of CSID symptoms.2 A small number of patients may require hospitalization for diarrhea and dehydration, malnutrition, muscle wasting and weakness.1-3 Patients with confirmed CSID commonly report being examined in the past for toddler’s diarrhea, irritable bowel syndrome-diarrhea (IBS-D), lactose intolerance, celiac disease, cystic fibrosis, or food allergies.1,4
The gastrointestinal (GI) symptoms associated with CSID tend to persist in adults, because CSID is not a disease that a patient can outgrow. Symptoms may appear less severe in adults compared to those experienced by children. In some adults, symptoms may be limited to an increase in bowel movement frequency, abdominal distention, and flatulence. Episodic watery diarrhea upon ingestion of high levels of sucrose may occur.1 In certain patients, diarrhea may alternate with constipation, leading to a misdiagnosis of CSID as irritable bowel syndrome-alternating (IBS-A).
As with pediatric patients, the clinical presentation in adults varies dramatically from patient to patient. Some patients with CSID may experience several severe symptoms in response to consumption of sucrose, while others may experience only mild discomfort.
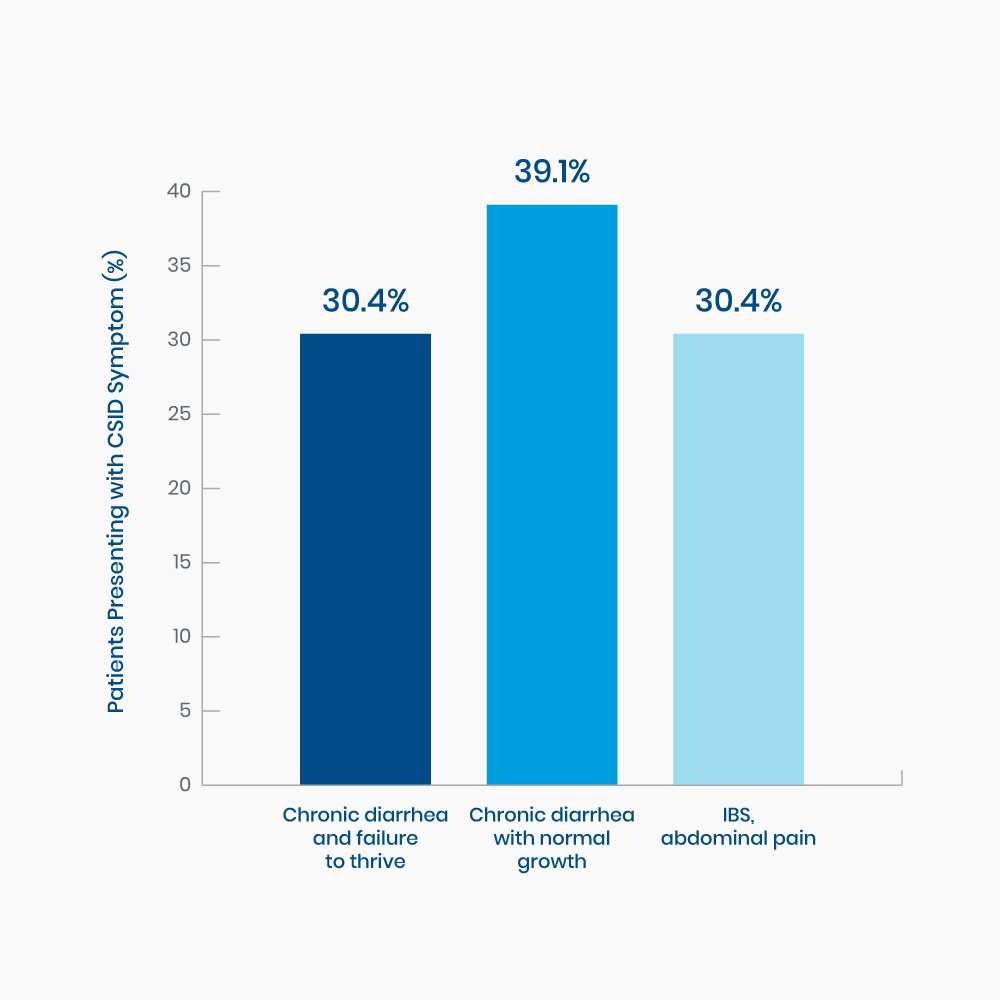
Figure 1. Distribution of presenting symptoms of CSID in twenty-three pediatric patients1
Symptoms Consistent with a Diagnosis of CSID
Table 1. Overview of CSID Symptoms
Common Signs and Symptoms
Individuals with Congenital Sucrase-Isomaltase Deficiency (CSID) typically have one or more of the following symptoms:
- Chronic diarrhea and/or loose stools (more severe or explosive in young children or babies after they have stopped breastfeeding)
- Acidic stools (stool pH <6) resulting in excoriated buttocks or rash
- High frequency of bowel movements (BMs)
- Reports of particularly foul BM odor related to poor absorption of carbohydrates
- Gas and abdominal bloating
- Abdominal pain
- Complaints of nausea or indigestion
- Diarrhea mixed with intermittent constipation, particularly when chronically taking common drugs to stop diarrhea
- Onset of symptoms soon after consuming a meal
- A low body mass index (BMI) that falls below the age-appropriate growth chart curve or failure to thrive when very young
- Avoidance or intolerance of foods containing carbohydrates, particularly sugary sweets or starches (for example, potatoes, rice, pasta)
- Lack of relief from treatment with common drugs to stop diarrhea
- Long history of examinations by multiple gastroenterologists for unusual GI conditions with symptoms similar to CSID, such as inflammation of the gall bladder (cholecystitis); intolerance of foods containing gluten (proteins found in grains), called celiac disease; an inherited disorder that impairs the secretion of mucus, called cystic fibrosis; and impaired absorption of bile acid (naturally-occurring molecule that helps the body break down fats); all these conditions also may cause chronic diarrhea
Family History of GI Symptoms
Since CSID is an inherited disorder, other family members may also be affected:
- Parents and/or siblings may have similar GI symptoms after a meal
- They may avoid eating carbohydrates and sweet foods
Symptom Frequency and Duration
- Individuals with CSID may experience GI symptoms frequently (several times a week or every day)
- Onset of symptoms is shortly after eating a meal
- Symptoms have been a problem for a very long-time (since childhood or for many years); in children, symptoms may start when no longer breastfeeding, with increased consumption of dietary carbohydrates in baby foods
References
- Treem WR. Congenital Sucrase-Isomaltase Deficiency. J Pediatr Gastroenterol Nutr. 1995;21(1):1-14. doi:10.1097/00005176-199507000-00001
- Gudmand-Høyer E. Sucrose malabsorption in children: a report of thirty-one Greenlanders. J Pediatr Gastroenterol Nutr. 1985;4(6):873-877. doi:10.1097/00005176-198512000-00005
- Antonowicz I, Lloyd-Still JD, Khaw KT, Shwachman H. Congenital Sucrase-Isomaltase Deficiency. Observations over a period of 6 years. Pediatrics. 1972;49(6):847-853.
- Treem WR. Clinical aspects and treatment of Congenital Sucrase-Isomaltase Deficiency. J Pediatr Gastroenterol Nutr. 2012;55(suppl 2):S7-S13. doi:10.1097/01.mpg.0000421401.57633.9


